- Home
- keyboard_arrow_right Phelan Dental Seminars
- keyboard_arrow_right How Do You Treat A Non-Restorable Central Incisor In Your Practice? Immediate Vs Delayed Implant Placement -Part 1
How Do You Treat A Non-Restorable Central Incisor In Your Practice? Immediate Vs Delayed Implant Placement -Part 1
Dr. Jim Janakievski September 6, 2011

In the last blog I presented a patient that had a non-restorable maxillary central incisor. She was treated with an immediate post-extraction implant placement and a custom provisional crown to immediately support the soft tissues.
Unfortunately, we can not always provide this form of treatment to all patients. When should we separate treatment into phases?
I had mentioned that we must take into consideration the shape and dimensions of the labial bone, the existing soft tissue profile and the amount of apical bone.
Immediate post-extraction implant placement requires ideal bone volume. The immediate implant is anchored into the apico-palatal bone. If the bone is this area is compromised, then implant stability may not be achievable. In addition, the bone on the facial supports the soft tissue profile. Thin bone or large dehiscences are a risk for future gingival recession. A patient with inadequate facial alveolar bone should not receive an immediate implant.
This next patient I will present also had a non-restorable failing maxillary central incisor. As a teenager, this tooth was traumatized during a sports injury. It was endodontically treated and crowned. Ten years later, this tooth required apical endodontic surgery. The patient is now 40 years old, and presents with a fistula at the apex of the central incisor. The patient consulted with members of our team, including an endodontist. After reviewing his options, he requested to have this tooth replaced with a dental implant.
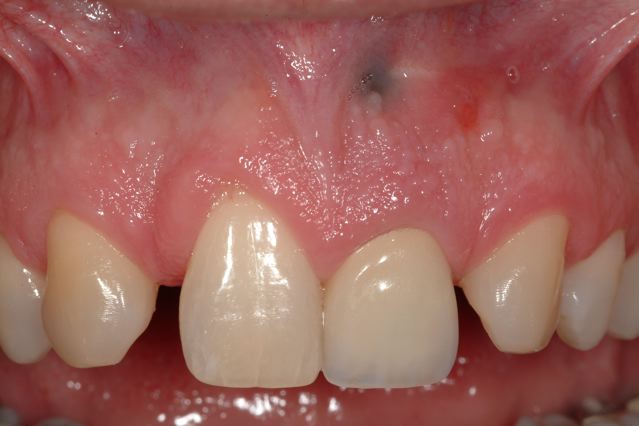
From the clinical exam, we can determine that the soft tissue profile for this failing tooth is more coronal than the adjacent central incisor, which has slight gingival recession.
We have a very favorable soft tissue position prior to surgery, so soft tissue augmentation may not be necessary.
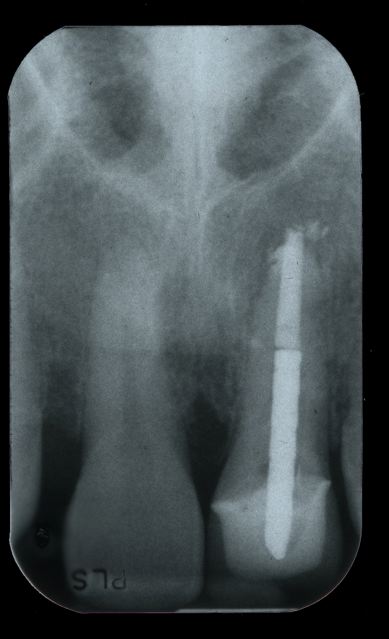
Further clinical evaluation we note a fistula at the apex of #9(FDI #21). On the radiographs, we determine that there is a peri-radicular lucency that extends to the floor of the nose. Since this is the area that I depend on for implant stability, it is unlikely that I can predictably place the implant at the time of extraction.
So how should we manage this site? How do we extract, debride and graft the alveolar ridge?
My approach follows a sequence of steps, intended to both correct and maintain the alveolar dimensions.
After extraction, I observed that the crestal bone on the facial aspect of the socket was intact and at a favorable level. However, the lesion had resorbed the overlying bone in the apical zone.
So to gain good access to the lesion, I made a C-shape incision around the apical fistula. In addition, this allowed access for placement of the bone graft and membrane. By avoiding flap reflection in the crestal half of the ridge, I was able to maintain the blood supply to the alveolar facial bone. The ridge was grafted with allograft bone and the socket closed with an epitheliazed graft.
In the next blog, we will discuss implant placement and restoration.
Note Large Apical Lucency
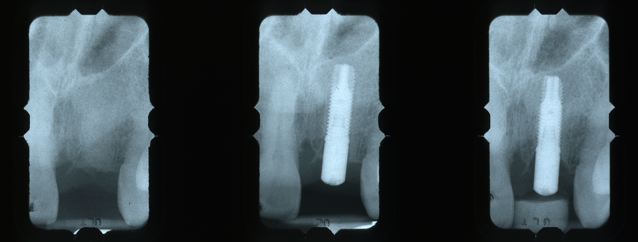
Interproximal Bone Adjusted At Time Of Surgery To Provide Room For Future Restoration
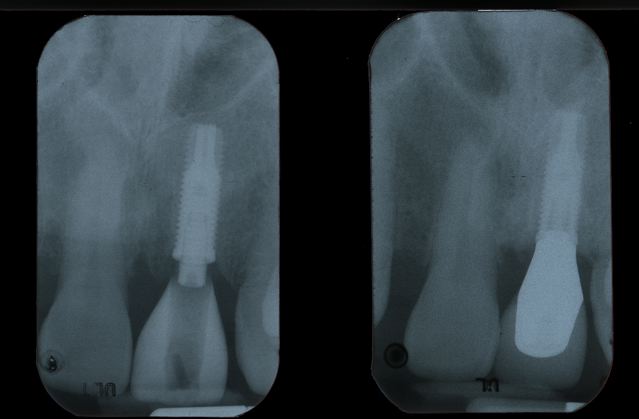
Provisional And Final Restoration
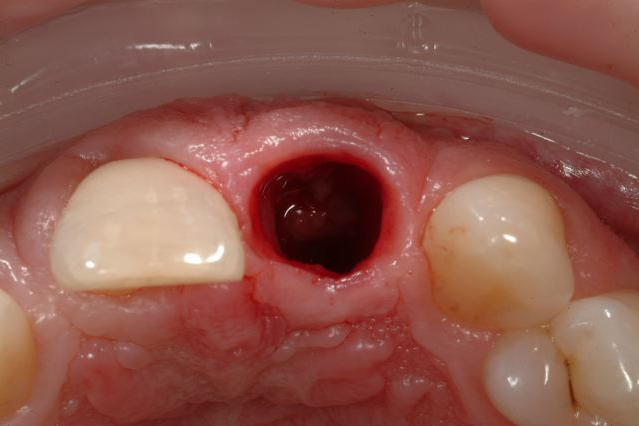
Initial Presentation
Occlusal View Of Socket
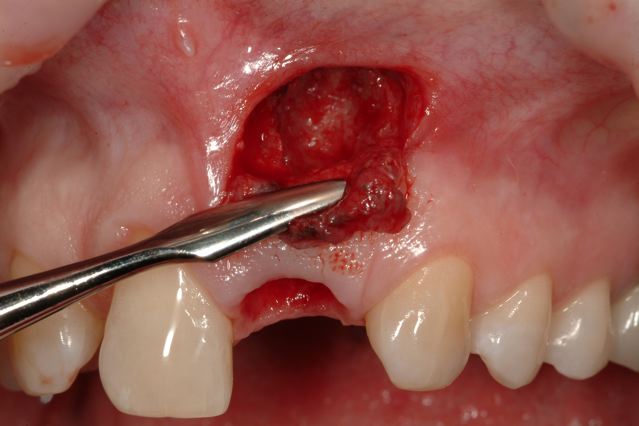
Apical Lesion Debrided
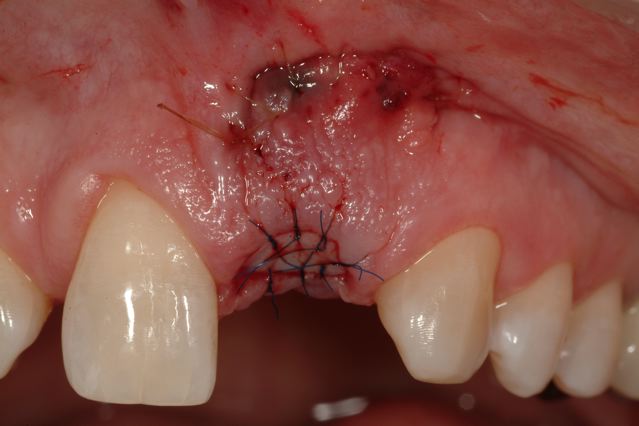
Alveolar Grafting Completed
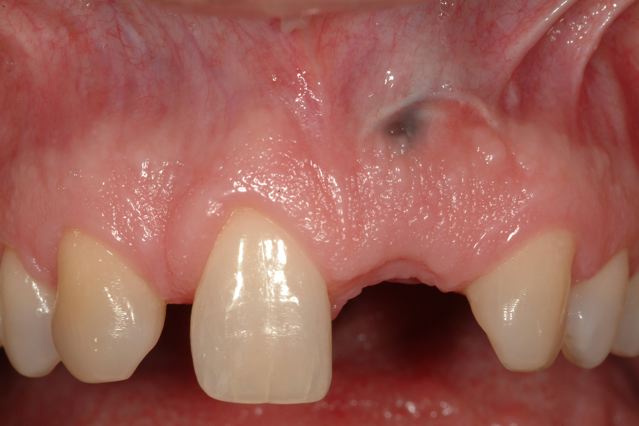
Alveolar Ridge Graft Healed
Tagged as: Dr. Stephen Phelan, immediate, delayed, immediate provisional, Janakievski, Dr Jim Janakievski, Phelan.
Post comments (1)
© Copyright Phelan Dental Seminars I Dr. Stephen Phelan



samsung galaxy a3 review pc pro on November 9, 2016
The great thing is t it supports for HTML web surfing on account of the Opera Mini that
is pre-installed in this device. This is a similar kit
as based in the desired Beats headsets that are fast replacing the iconic white i – Pod headsets
if you’re inside their gadgets. It is powered
from the latest Cortex A9 core 1GHz MT6575 processor that could generate efficient management of the resources.