- Home
- keyboard_arrow_right Phelan Dental Seminars
- keyboard_arrow_right Interesting Worn Dentition Case Part 2

Hi everyone,
I wanted to start off by thanking all of you for the excellent ideas and comments related to my last post. Many of you had excellent thoughts about how this wear evolved over the years and how you would help this patient. Today I would like to share with you the etiology of the wear and the actual treatment plan that the patient selected.
As I stated in the last post this particular patient came into my practice with a significant amount of tooth wear but he had no TMJ or muscle symptoms and has good bone levels around his teeth.
There are a number of correct answers to the question I asked about the etiology of wear for a patient like this and if you look in the comments section of the first post you will see many great ideas from the people that participated.
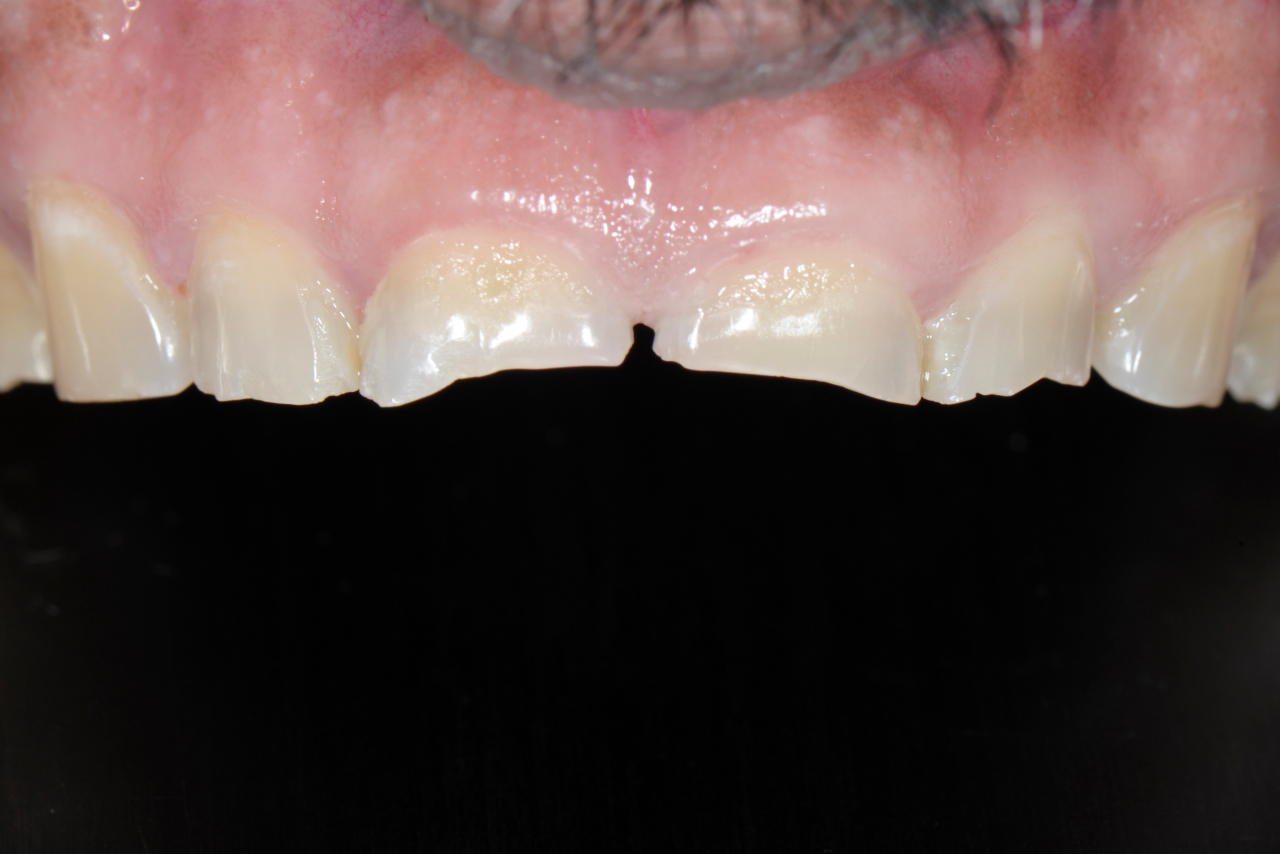
Examination of the tooth wear revealed that the wear facets were present on tooth surfaces that were not in occlusal contact. Attrition requires the wear to be derived from tooth to tooth contact so this wear appears to be predominantly from erosion.
This patient was aware that he had significant wear and when questioned about the etiology he let us know that he consumed one 1.5 liter bottle of Coca-Cola per day for the last 20 years. With a pH of 2.48 Coca-Cola consumption of this magnitude and duration would certainly lead to this amount of erosion and tooth loss.
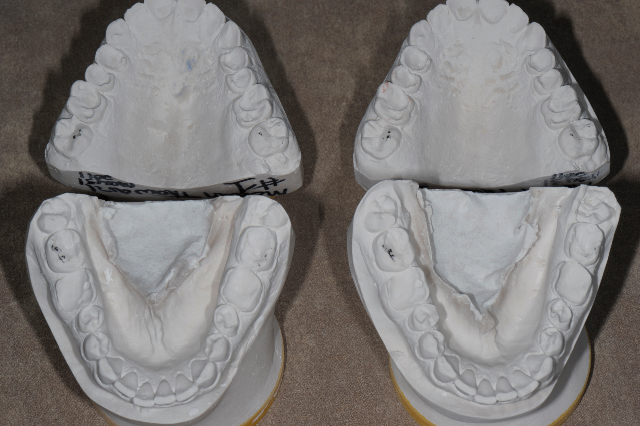
During the functional analysis large centric relation interference was discovered on the palatal cusp of 17 and the buccal cusp of 47. This interference was also located and verified with the 2 sets of the CR mounted study models that were made with the 2 CR bite records. I take 2 sets of CR bite records and make 2 mountings to verify the accuracy of the bite records and the mountings. I am looking for the 2 sets of bite records and the 2 sets of mountings to be the same.
I then verify that the point of initial contact on the mountings matches what I found in the mouth. If all of this is consistent then I feel that the CR bite records and the mountings are accurate and can be used for the diagnostic wax-up.
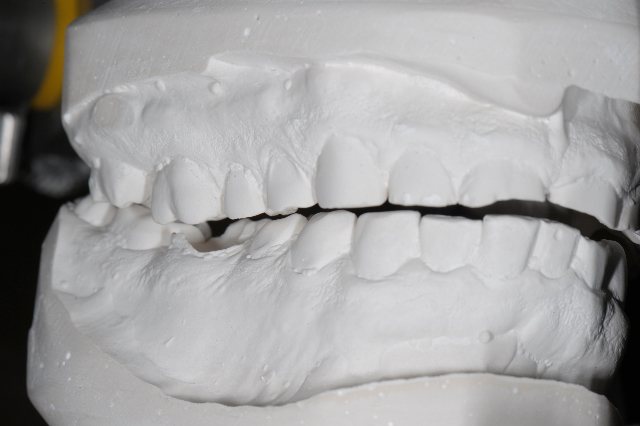
As you can see with the photograph of the 2 sets of mountings they match each other and the point of initial contact that I found during the functional analysis.
For this case the patient recognized that he needed significant restorative dentistry to be restored to a more healthy functional and aesthetic condition. He did ask if I could figure out a treatment plan that would fit within a reasonable budget and avoid a full mouth rehabilitation. With this in mind I treatment planned to open the vertical dimension to the point of initial contact and restore the upper arch from first molar to first molar and the first bicuspids and first molars on the lower arch. This treatment plan would lead to a 16 unit partial rehabilitation and I planned to use direct composite bonding to restore any erosion that is present in the remaining dentition.
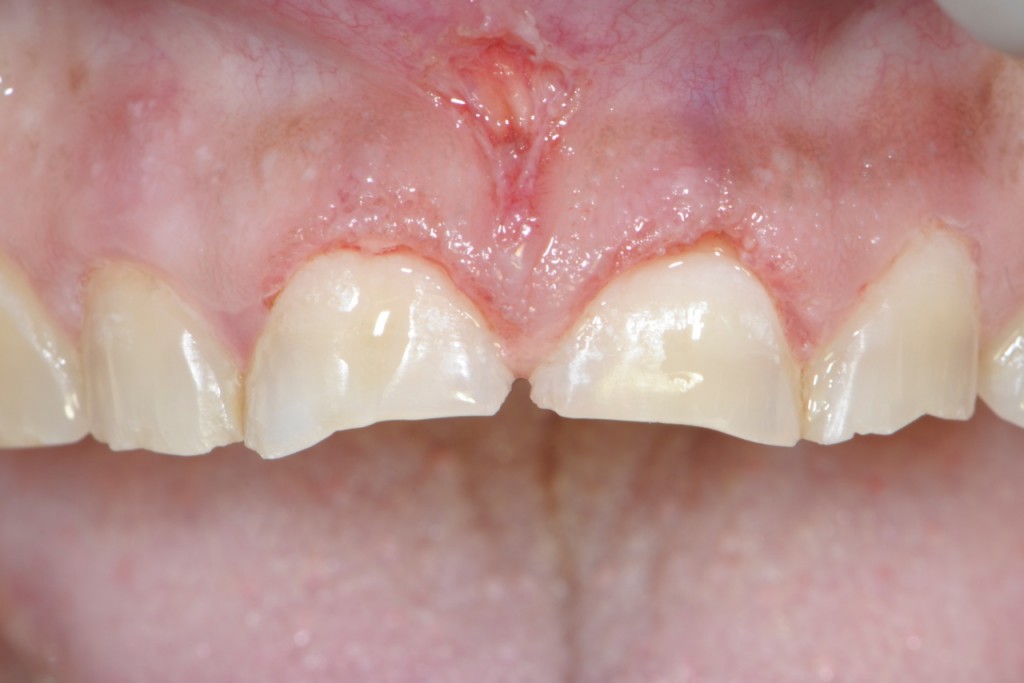
I also planned to alter the gingival levels of 11 (8) and 21 (9) to improve the gingival symmetry as well as the retention and resistance form.
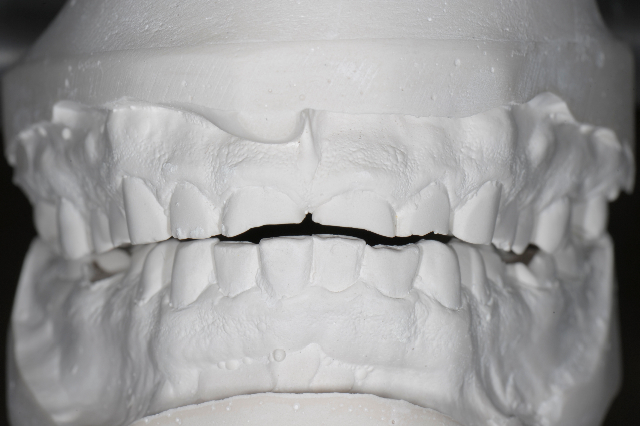
If you place the study models from this case on the Sam 3 articulator and close to the point of initial contact you can see the vertical dimension that the case will be waxed up to. This technique will open the vertical dimension in most cases more than enough for the restorative material requirements without increasing the contracted length of the elevator muscles.
For this patient with his MI position he had no room for the restorative material due to extensive erosion and tooth eruption that has led to an end-to-end anterior tooth relationship. If you tried to restore him to his MI position you would compromise the structural integrity of the upper anterior teeth. This can be solved with either orthodontics or opening his vertical dimension.
I have completed the crown lengthening with my Waterlase MD dental laser and the case is now being waxed up with the initial preparations scheduled in 3 weeks. I hope these posts have provided you with some interesting ideas about treating this type of case. As usual you can add any questions or comments using the link above.
Anterior Teeth Before Gingival Adjustment
Anterior Teeth After Gingival Adjustment With The Waterlase MD Laser
2 Sets Of Mounted Models
Models At The Point Of Initial Contact
Models At The Point Of Initial Contact
Models At The Point Of Initial Contact
Models At The Point Of Initial Contact
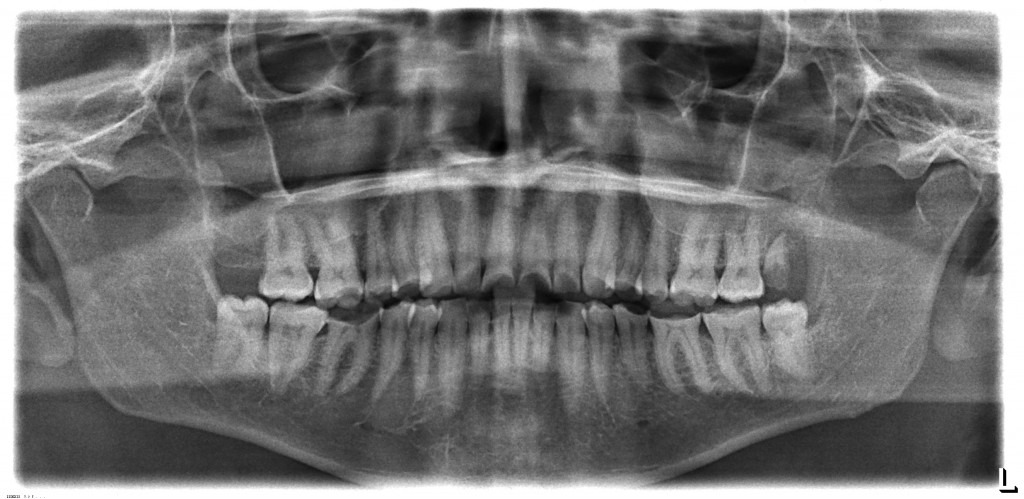
Panorex
Post comments (6)
© Copyright Phelan Dental Seminars I Dr. Stephen Phelan




Mike on July 7, 2011
Thanks for sharing this case Stephen – Beautiful pictures as usual.
Do you retake the study model impressions for the diagnostic waxup after the crown lengthening, or do you send out the initial models to the lab? It looks like you did a bit of a maxillary frenectomy as well with the esthetic crown lengthening. How long do you normally wait after soft tissues procedures before taking final impressions?
Dr Stephen Phelan on July 8, 2011
Hi Joe,
It is close and thermal sensitive but tested vital. Time will tell if it needs endodontic treatment but I will leave the patient in provisional restorations for a few months to see how it responds.
Dr Stephen Phelan on July 8, 2011
Hi Mike,
Yes I decided to do a frenectomy at the same time as the gingivectomy. The healing time really depends on the type of procedure. With a gingivectomy using a laser if you are not going to invade the biologic width and remove bone I will let it heal for about 4 weeks. If you need to do a flap and osseous surgery I would wait at least 3 months.
Remember to sound to the osseous crest and make sure you do not invade the biologic width before a gingivectomy.
I will often take a new set of study models after the gingival alteration for the diagnostic wax up and mount them with the original bite records. We keep all the bite records in case we decide to do this.
Arnie Mirza on July 9, 2011
Hi Dr. Phelan
Thank you for such a nice and interesting case.I have done such few cases with generalized wear down with direct composite using a suction down form on models done for the wax-up, for sure taking imp for the wax-up. It works very well but the only disadvantage is to floss using a threader or to separate the contacts with a disc. So Dr. Phelan which way are you using? Do you use CAD/CAM to mill the resin restoratins? Thank you.
Gary Guy on July 13, 2011
Diagnosed as a computer illiterate by my boss who has purchased my practise( 1974- 2010) one of the conditions of the sale was to give something back. I am to put together a series of presentations to his peers on how to do a full mouth reconstruction 2-4-8-16 teeth at a time.Your articles have me keeping you as a potential mentor as I have been trying to reproduce CR from the late 70’s to the present starting with- PKThomas , Pete Dawson, Tom Basta ( F.A.C.E.) , with continuing support from Kois, Spier, and a bunch of us who choose to start from the inside out. I have 6 SAM 2’s with cross references to 3 labs and recently realized Sam 2 is dead! Your article on how to reproduce consistent CR recordings is what I have been doing for most of my career and this is why I am trying to be more computer literate. My students will have to be up to date and your article on what it is that I’ve been trying to be doing looks like it can carry on with the SAM 3. If you are interested in helping with my last pursuit in giving something back to our profession I look foreword to keeping in touch.
Garry
(PS) I have a Stuart Articulator with Denar a Pantographic Recording apparatus for inside out mentality so you can do PDG Tripodisation . Want to buy it?
Joe Bulger on July 7, 2011
That #46 (30) looks scary close to the pulp. Any teeth symptomatic?